Abstract
Objective
To improve the usage of expressed breast milk in very low birth weight infants admitted in the neonatal intensive care unit of a tertiary centre in India.
Methods
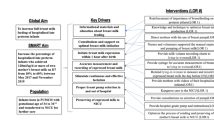
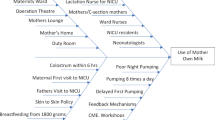
Between April 2015 and August 2016, various Plan-do-act-study cycles were conducted to test change ideas like antenatal counselling including help of brochure and video, postnatal telephonic reminders within 4–6 hours of birth, standardization of Kangaroo mother care, and non-nutritive sucking protocol. Data was analyzed using statistical process control charts.
Results
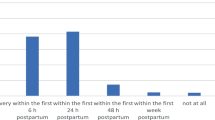
156 very low birth weight infants were delivered during the study period, of which 31 were excluded due to various reasons. Within 6 months of implementation, the proportion of very low birth weight infants who received expressed breast milk within 48 hours improved to 100% from 38.7% and this was sustained at 100% for next 8 months. The mean time of availability and volume of expressed breast milk within 48 hours, improved gradually from 73.3 h to 20.9 h and 4.7 mL to 15.8 mL, respectively. The mean proportion of expressed breast milk once infant reached a feed volume of 100 mL/kg/day also improved from 61.3% to 82.3%.
Conclusion
Quality improvement interventions showed promising results of increased expressed breast milk usage in very low birth weight infants.
Similar content being viewed by others
References
Henderson G, Anthony MY, McGuire W. Formula milk versus maternal breast milk for feeding preterm or low birth weight infants. Cochrane Database Syst Rev. 2007;17:CD002972.
Meier PP, Engstrom JL, Patel AL, Jegier BJ, Bruns NE. Improving the use of human milk during and after the NICU stay. Clin Perinatol. 2010;37:217–45.
Schanler RJ, Lau C, Hurst NM, Smith EOB. Randomized trial of donor human milk versus preterm formula as substitutes for mothers’ own milk in the feeding of extremely premature infants. Pediatrics. 2005;116:400–6.
Schanler RJ, Shulman RJ, Lau C. Feeding strategies for premature infants: Beneficial outcomes of feeding fortified human milk versus preterm formula. Pediatrics. 1999;103:1150–7.
Vohr BR, Poindexter BB, Dusick AM, McKinley LT, Higgins RD, Langer JC, et al. Persistent beneficial effects of breast milk ingested in the neonatal intensive care unit on outcomes of extremely low birth weight infants at 30 months of age. Pediatrics. 2007;120:e953–9.
Vohr BR, Poindexter BB, Dusick AM, McKinley LT, Wright LL, Langer JC, et al. Beneficial effects of breast milk in the neonatal intensive care unit on the developmental outcome of extremely low birth weight infants at 18 months of age. Pediatrics. 2006;118:e115–23.
Battersby C, Santhakumaran S, Upton M, Radbone L, Birch J, Modi N, et al. The impact of a regional care bundle on maternal breast milk use in preterm infants: outcomes of the East of England quality improvement programme. Arch Dis Child Fetal Neonatal Ed. 2014;99:F395–401.
Sisk PM, Lovelady CA, Dillard RG, Gruber KJ. Lactation counseling for mothers of very low birth weight infants: effect on maternal anxiety and infant intake of human milk. Pediatrics. 2006:117:e67–75.
Murphy L, Warner DD, Parks J, Whitt J, Peter-Wohl S. A quality improvement project to improve the rate of early breast milk expression in mothers of preterm infants. J Hum Lact. 2014;30:398–401.
Pineda RG, Foss J, Richards L, Pane CA. Breastfeeding changes for VLBW infants in the NICU following staff education. Neonatal Netw. 2009;28:311–9.
Ward L, Auer C, Smith C, Schoettker PJ, Pruett R, Shah NY, et al. The human milk project: a quality improvement initiative to increase human milk consumption in very low birth weight infants. Breastfeed Med. 2012;7:234–40.
Meier PP, Engstrom JL, Mingolelli SS, Miracle DJ, Kiesling S. The Rush Mothers’ Milk Club: breastfeeding interventions for mothers with very-low-birth-weight infants. J Obstet Gynecol Neonatal Nurs. 2004;33:164–74.
Verma A, Maria A, Pandey RM, Hans C, Verna M, Sherwani F. Family-centered care of sick newborns. A randomized controlled trial. Indian Pediatr. 2017;54:453–9.
Dogra S, Thakur A, Garg P, Kler N. Effect of differential enteral protein on growth and neurodevelopment in infants <1500 g: A randomized controlled trial. J Pediatr Gastroenterol Nutr. 2017;64:e126–e32.
Amin SG. Control charts 101: A guide to health care applications. Qual Manag Health Care. 2001;9:1–27.
Benneyan JC, Lloyd RC, Plsek PE. Statistical process control as a tool for research and healthcare improvement. Qual Saf Health Care. 2003;12:458–64.
Moen RD, Nolan TW, Provost LP. Improvement in Quality In: Judy Bass, editor. Quality Improvement through Planned Experimentation, 3rd ed. New York: McGraw-Hill; 2012.p. 1–23.
Provost LP, Murray SK. Learning from Variation in Data In: Jossey Bass, editors. The Healthy Care Data Guide Learning from Data for Improvement, 1st ed. San Francisco: Wiley Inc; 2011. p. 116–7.
Spatz DL. Ten steps for promoting and protecting breastfeeding for vulnerable infants. J Perinat Neonatal Nurs. 2004;18:385–96.
Fugate K, Hernandez I, Ashmeade T, Miladinovic B, Spatz DL. Improving human milk and breastfeeding practices in the NICU. J Obstet Gynecol Neonatal Nurs. 2015;44:426–38.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thakur, A., Kler, N., Garg, P. et al. Impact of Quality Improvement Program on Expressed Breastmilk Usage in Very Low Birth Weight Infants. Indian Pediatr 55, 739–743 (2018). https://doi.org/10.1007/s13312-018-1371-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-018-1371-8